Over 200,000 people newly diagnosed with chronic kidney disease over four years
Sign up now: Get ST's newsletters delivered to your inbox
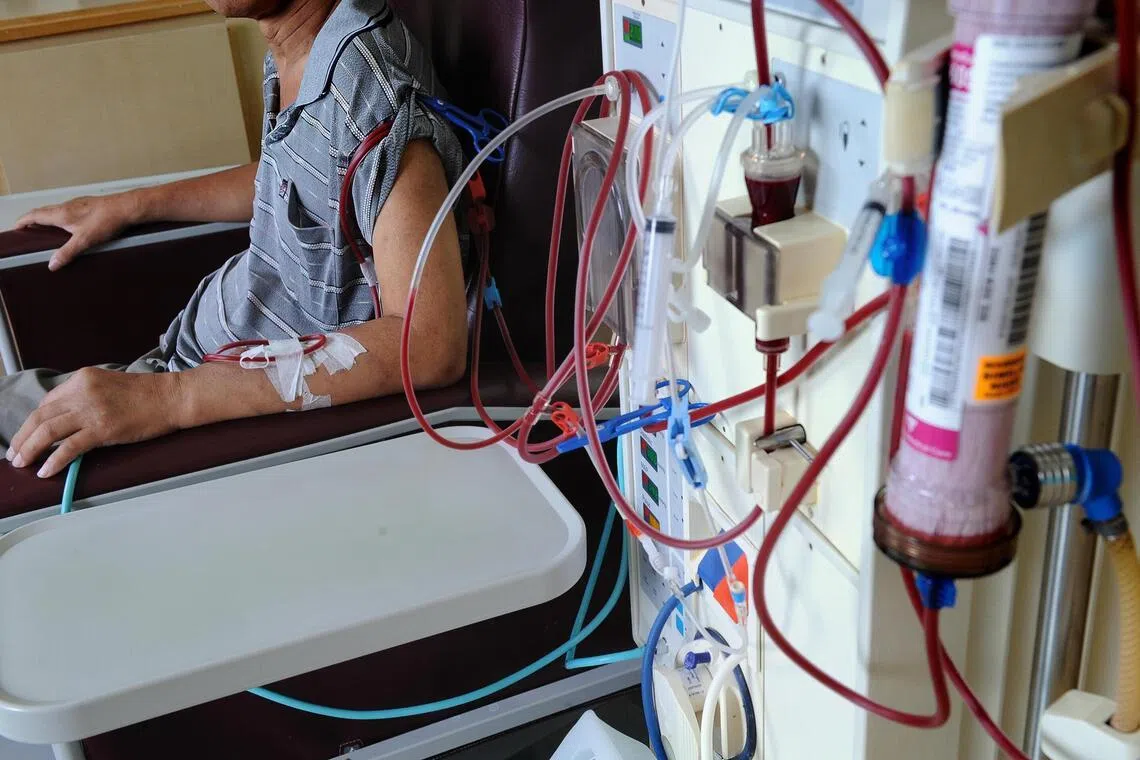
More than 200,000 residents were newly found over four years to have chronic kidney disease, which could lead to a surge in demand for dialysis services in the future..
ST PHOTO: DESMOND WEE
SINGAPORE – More than 200,000 residents in Singapore were newly found over a span of four years to have signs of impaired kidney function. About 1,000 Healthier SG clinics outside the public healthcare sector have been tapped to monitor and care for these patients.
This move by the Ministry of Health (MOH) hopes to prevent these patients’ condition from worsening, which could cause a potential surge in the country’s dialysis burden.
Among Singapore residents between 18 and 74 years old, after adjusting for age differences, the rate of those who have chronic kidney disease (CKD) increased to 13.9 per cent during the period of 2023 to 2024.
This is nearly 60 per cent higher than the 8.7 per cent for 2019 to 2020, according to the latest National Population Health Survey (NPHS) findings released by MOH in October 2025.
Survey respondents had their blood and urine samples collected and analysed.
Health Minister Ong Ye Kung said in March 2026 that despite the prevalence of diabetes and high blood pressure staying broadly stable, the absolute numbers of people with CKD and requiring dialysis continued to rise as more Singaporeans are older and more susceptible to CKD.
CKD refers to the long-term condition of irreversible damage to the kidneys, with a gradual loss of their filtering ability.
CKD is usually brought about by risk factors such as hypertension (high blood pressure) and diabetes.
There are five stages of CKD. Dr Jason Choo, medical director of the National Kidney Foundation (NKF), said stage 1 means there is some kidney damage, such as the presence of protein in the urine, but the organ is still functional.
Stage 5 is end-stage renal disease, also known as kidney failure, where dialysis or a kidney transplant may be required.
Since 2017, MOH has implemented the Holistic Approach in Lowering and Tracking Chronic Kidney Disease (HALT-CKD) programme across all public healthcare institutions, with the aim of slowing the progression of CKD.
Preventive efforts have since expanded to private healthcare, with MOH roping general practitioners (GPs) into the Healthier SG programme to care for patients with CKD. As at February 2026, there were about 1,100 Healthier SG clinics.
MOH implemented care protocol for these GPs in January 2025, to provide guidance.
Dr Jonathan Yeo, a director of Family Medicine Clinic Chinatown, said the guidance helped GPs manage patients with mild and moderate CKD and appropriately refer more complex cases to kidney specialists.
The senior family physician has been co-chairing the Healthier SG Care Protocols Sub-Workgroup since July 2023. This group oversaw and facilitated the drafting and refinement of various Healthier SG care protocols.
Before the launch of the CKD care protocol, there were local guidelines on CKD care and all three polyclinic clusters had their own set of guidelines.
What the care protocol did was to consolidate the key approaches and principles, giving GPs a uniform approach to managing those with CKD, said Dr Yeo.
Nearly 60 per cent increase highlighted potential strain on healthcare system
The increase in CKD prevalence was “not statistically significant”, stated MOH in the NPHS report.
Nonetheless, NKF’s Dr Choo was of the view that this was still important from a public health perspective, as it highlighted the potential strain on the healthcare system should more cases progress to advanced disease if their CKD was not detected or well managed.
He said the increase in prevalence translated to more than 200,000 residents between 18 and 74 newly diagnosed with CKD, bringing the total to an estimated 500,000.
The actual health burden is likely to be higher as those who are older face a higher CKD risk, but they are not covered under the scope of NPHS, added Dr Choo.

Dr Jason Choo, medical director of the National Kidney Foundation, said the actual number of people newly diagnosed with chronic kidney disease could be more than 200,000.
PHOTO: THE NATIONAL KIDNEY FOUNDATION
He noted that even if a small proportion, say 5 per cent, of these 500,000 patients eventually require dialysis after kidney failure, this would amount to about 25,000 new patients – more than double the 10,000 now on dialysis in Singapore.
In the light of the latest NPHS results, The Straits Times asked MOH to comment on the effectiveness of the HALT-CKD programme in slowing patients’ CKD progression.
MOH said in its reply: “As the implementation of CKD care through Healthier SG GPs started recently in 2025, MOH will continue to review its effectiveness and progress over the next few years.”
Efforts in place to tackle growing health concern
Moves have been made to tackle the risk factors of CKD, such as diabetes and hypertension, including upstream measures of promoting healthier lifestyles and diets, said Senior Minister of State for Health Tan Kiat How in November 2025, at the opening of a SATA CommHealth dialysis centre in Fernvale.
Describing CKD as a “growing health concern” in Singapore, he noted that like many chronic conditions, it progresses silently and can occur at the same time as other chronic conditions.
“This makes early detection and management critical, which is why under Healthier SG, an annual kidney assessment is mandatory as part of recommended care” for those with diabetes and hypertension, said Mr Tan.
In its reply to ST, MOH said that as of March 2024, HALT-CKD has enrolled more than 110,000 patients with CKD in polyclinics and other public healthcare institutions.
More than 80 per cent of the patients have been prescribed kidney protective medication, including newer drugs such as sodium-glucose cotransporter-2 inhibitors, which have been shown to prevent a decline in kidney function.
Patients are also monitored for blood glucose control because poorly controlled diabetes is a risk factor for progression to end-stage renal disease.
Other risk factors, such as smoking and comorbidities – medical conditions that occur at the same time as other conditions – such as hypertension, are monitored and managed too.
The NPHS results showed that the prevalence of CKD among those with both diabetes and hypertension was 47.4 per cent – higher than that of those with only diabetes (34.4 per cent), with only hypertension (21.4 per cent), and without either of the chronic diseases (6.3 per cent).
Both Dr Choo and Dr Yeo emphasised the importance of early detection and regular monitoring.
On this front, NKF is working on kidney screening in the community. To date, more than 200 GP clinics have screened more than 9,000 at-risk individuals, with around one in seven requiring further follow-up.
Dr Yeo raised an example of how patients tend to view each chronic condition as a stand-alone condition and fail to appreciate that poor control of blood sugar or high blood pressure will weaken their kidney function.
“By the time they realise their kidneys have been significantly weakened, the damage is no longer reversible,” he said.
He also said many people have a preconceived notion that there must be “pain in the kidneys or the back” to signify deteriorating kidney function or a kidney problem.
However, CKD is largely asymptomatic until the patient reaches end-stage kidney failure, so the mentality of “no symptoms means I must be healthy” is erroneous, said Dr Yeo.


